By: Donovan Martin Sr, Editor in Chief
There are treatments that feel like rescue, and there are others that feel like a negotiation with time, and dialysis exists in that uneasy space where medicine is no longer restoring the body but stepping in to partially replace what has been lost. When the kidneys fail, toxins build, fluid accumulates, and the chemistry of the body begins to drift into dangerous territory, and what follows is not optional because without intervention the body cannot sustain itself for long. What is often presented as a necessary next step is, in reality, the beginning of a fundamentally different way of living, one that is structured, controlled, and in many cases permanent.
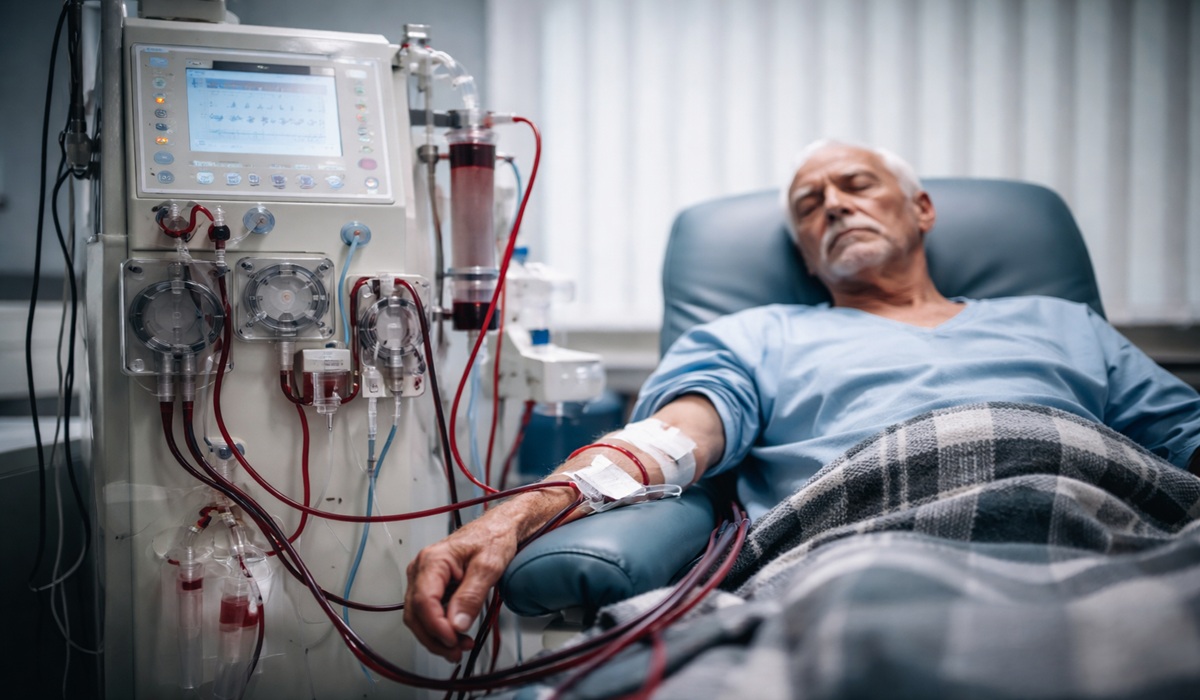
The process itself is far more invasive and physically demanding than most people fully grasp at the outset, because it is not simply a matter of being connected to a machine but rather a repeated mechanical intervention into the bloodstream. Blood is drawn out of the body through a surgically created access point, typically in the arm where a vein and artery are joined to handle the volume and pressure required, and that blood is then pushed through a filtration system that removes waste, toxins, and excess fluid before being returned back into circulation. This cycle continues for hours at a time, several times a week, and it relies on precision, pressure, and constant monitoring, because even small imbalances can create complications. The body, which once performed this function silently and continuously, is now dependent on an external system that replicates it imperfectly and intermittently.
What happens during those hours is only part of the story, because the effects extend well beyond the treatment chair and into the rest of the patient’s life. Many experience significant drops in blood pressure, which can lead to dizziness, nausea, and a level of exhaustion that does not simply pass after rest, while others deal with muscle cramping as fluid is removed faster than the body can comfortably adapt. Over time, the repeated strain of treatment can place additional stress on the cardiovascular system, while the access point itself becomes a permanent vulnerability that must be maintained and monitored. This is not a temporary intervention that fades into the background, but a continuous, invasive routine that reshapes both the body and the rhythm of everyday life.
For some patients, that trade is worth it, because it offers more time, more experiences, and more opportunities to remain present for the people and moments that matter most. There are individuals who adapt to the routine, who build their lives around it, and who find a way to maintain a sense of normalcy within the constraints. But there is another reality that develops alongside this one, and it is far less openly discussed, because not every patient experiences that time as meaningful in the same way.
There are many who reach a point where the treatment begins to feel less like an extension of life and more like the management of decline, where the energy required to endure the process begins to outweigh what they are able to get out of the days in between. The fatigue compounds, the hospital visits become more frequent, and the sense of independence slowly erodes, not all at once but gradually enough that it is easy to miss until it becomes undeniable. What began as a life-sustaining intervention can, for some, evolve into a cycle that sustains the body while narrowing the experience of living.
That cycle carries a psychological weight that is often underestimated, because life becomes structured around appointments, recovery time, and the knowledge that missing even a single session carries serious consequences. There is very little room for spontaneity, and even small disruptions can create stress that extends beyond the physical. Over time, that dependency can reshape how a person sees themselves, because they are no longer simply living with a condition, but living within a system that dictates the terms of their survival.
In speaking with a medical professional who has spent decades working in this field, someone widely respected and deeply experienced, what comes through is not detachment but a strong sense of responsibility and care. This is not someone who views patients as numbers or outcomes, but as individuals navigating incredibly difficult circumstances, and that perspective is grounded in both knowledge and lived experience. There is a clear commitment to the Hippocratic oath, not as a concept, but as something actively carried into daily practice, where every decision is weighed against what is truly in the patient’s best interest.
At the same time, that experience has exposed them to a reality that cannot be ignored, because they have seen firsthand the patients who struggle with the process, who openly question whether what they are enduring is giving them a quality of life they recognize as their own. These are not rare conversations, and they are not dismissed lightly, because they come from people living inside the reality of treatment, not observing it from the outside. When those perspectives are shared by someone with that level of medical insight and long-term exposure, it becomes difficult to simply default to the assumption that continuation is always the correct path.
This is where the conversation becomes more complex, because the principle of doing no harm is not always as straightforward as it appears. It is easy to interpret that principle as a mandate to preserve life at all costs, but when a treatment sustains biological function while steadily diminishing the lived experience of the patient, the definition of harm becomes less clear and far more nuanced. It forces a deeper examination of whether continuing without reflection is always aligned with the intent of care, or whether, in some cases, it begins to move into a space where the line is no longer so easily defined.
The broader system in the United States adds another layer to this discussion, because it is built to sustain and deliver ongoing treatment at scale, and it does so with remarkable efficiency. Dialysis clinics have become a common presence across the country, accessible and consistent, designed to meet a growing and ongoing need. That level of infrastructure reflects both medical capability and demand, but it also introduces a dynamic that cannot be ignored, because when a treatment becomes continuous, standardized, and widely available, it also becomes part of a financial structure that is driven by volume.
Over time, the expansion of these clinics has followed that demand, but the question that follows is whether the demand itself is always fully examined or simply absorbed into the system. When continuation becomes the default, and when the system is structured to support that continuation indefinitely, it becomes more difficult to pause and ask whether every patient is being given a fully transparent understanding of what that path entails over the long term. This is not about assigning intent to individual practitioners, many of whom approach their work with integrity, but about recognizing that systems shape behavior, and that not all incentives are neutral.
For patients, the decision to begin dialysis is often made in moments of urgency, where the alternative is immediate and severe decline, and in those moments the focus is understandably on survival rather than long-term trajectory. As time passes and the routine becomes established, a different awareness begins to take hold, because what was initially presented as a necessary intervention becomes the defining structure of daily life. That structure often follows a progression, beginning with adjustment, moving into a period of relative stability, and then, for many, gradually shifting into increasing difficulty as complications and fatigue accumulate.
At that point, the question is no longer whether the treatment works in a technical sense, but whether it continues to align with what the individual considers a life worth living. This is where honest, ongoing conversations become essential, not as a last resort, but as a standard part of care that evolves alongside the patient’s condition. The decision to start is not the same as the decision to continue indefinitely, and treating it as though it is ignores the reality that circumstances change.
There are alternatives, though none are simple or universally available, because transplantation can offer a different path but is limited by access and eligibility, while conservative management focused on comfort rather than intervention is often introduced too late to be fully considered. Both options require the same level of transparency and discussion that the initial decision deserves, yet they are not always presented with equal weight or timing.
Family dynamics further complicate the situation, because patients are rarely making these decisions in isolation, and there is often an unspoken expectation to continue, to endure, and to fight for more time, even when the individual may feel differently. That pressure, while rooted in care and concern, can make it more difficult to have an honest conversation about what the patient truly wants, particularly when stopping treatment is framed as giving up rather than as a considered and personal choice.
What ultimately strengthens this entire discussion is not more technology, but more candor, because patients deserve to understand not only what dialysis does, but what it demands over time, and how it may reshape their lives in ways that are not immediately apparent. They deserve to be part of a conversation that is ongoing, not one that is concluded the moment treatment begins, and they deserve to feel empowered to reassess that decision as their circumstances evolve.
Dialysis is not a failure of medicine, but it is one of the clearest examples of its limits, because it can extend life without necessarily restoring the fullness of living, and it can offer time without defining what that time will feel like. The most forward-thinking approach is not to reject it, but to place it within a framework of intentional decision-making, where continuation is not automatic, but considered, revisited, and aligned with what matters most to the individual.
In the end, this is not a question that can be answered by systems, protocols, or machines, because it is not purely medical, but deeply human, and it asks something that each person must define for themselves. It asks whether the life being extended is still the life they want to live, and whether continuing remains an act of care, or something else entirely.